It’s finally over. 8 million of my little stem cells are now on ice awaiting transplant.
The harvesting procedure itself is done on an outpatient basis and is relatively simple as I’ll describe shortly. The hard work is done in the build up to it. 16 injections of granulocyte colony stimulating factor (or GCSF) are administered over 4 days to get the bone marrow into stem cell production hyperdrive to ensure enough are in the blood for harvest.
These injections are done 4 at a time; in my case, two in the belly and one in each arm. They can be done in 8, but you have a choice – 4 relatively painless injections a day, or 2 slightly more painful ones. I opted for the former. These are administered by a nurse that visits you at home or work and who has to take your pulse, temperature and blood pressure before and 30 minutes after to ensure all is OK. In my case, 2 days were in the Supreme Court and I remain thankful to the help the staff extended in finding a room for this to happen.
I have been mulling over whether to tell the “no holes barred” truth about the process, or whether to sugar coat it. The reason being is that I am unsure which will encourage more 16-30 year olds to sign up with Anthony Nolan. The truth may give people confidence that it isn’t that bad…… and it’s what I’ve opted for. The injections themselves don’t hurt. The first day is fine. But the side-effects come on Days 2, 3 and 4. There’s lethargy and fatigue – a kind of “can’t be bothered to do anything” feeling, which is then overlaid with bone pain. This is as a result of all that bone marrow being exercised hard…… it’s somewhere between the morning after having run a marathon and the aches and pains you get with flu. Moving helps, but it can interrupt sleep if it’s in certain places – I barely slept the night before Day 3 because it was all lower back pain. Thankfully it moved elsewhere afterwards, and paracetamol (the only drug you’re allowed to take to combat it) does help a bit. In rare cases, you can get other side effects, but you are closely monitored for them.
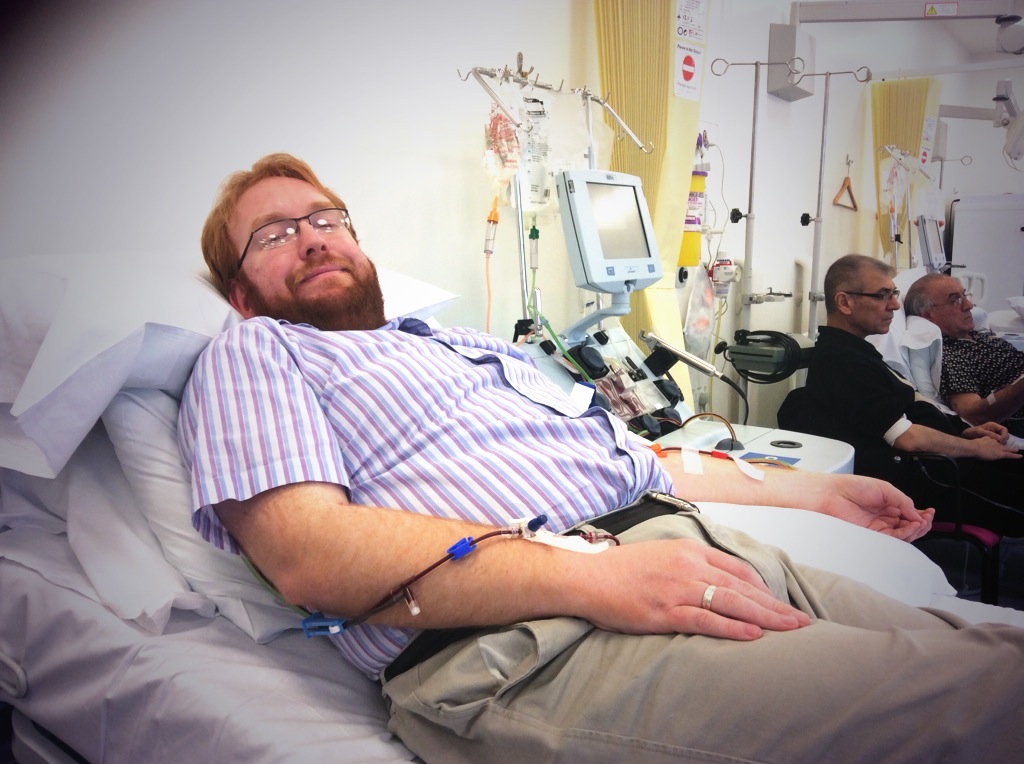
That then takes us to Day 5, the harvest. Courtesy of the tube strike I was late, but this was expected. You have a mini-medical with blood tests done in near real-time and settle down on a bed with a personal TV for company. A cannula is inserted into one arm – the dominant arm – this is no different to the type that you have for an operation, and it is where blood is returned to you. Then, a bigger needle is inserted into the other arm which is kept stretched out and immobile – it’s a long metal affair, so this restriction is to prevent damage to you, and is required to get your blood flowing out into the machine. I’ve always had problems with my veins; or rather medical professionals have always had problems getting them to play ball with their vampiric tendencies. This was no exception. A skilled nurse tried twice (there were two doses of local anaesthetic, so I barely felt a thing) but ended up having to call a specialist in for the third attempt – we were getting close to having a central line until he succeeded.
Thereafter, blood goes into the machine, gets centrifuged, the stem cell layer is extracted, the rest is returned to you. My entire blood volume was filtered twice. The greatest side effect at this stage is boredom and being subjected to day time TV. You have access to infinite coffee and biscuits – along with an NHS “lunch” and some banter with the staff – two of those three things are well appreciated!. At the end of the 5 hour collection process, the stem cells are whisked away and counted to ensure they have enough. They only needed 4m for my recipient (apparently she is a petite lady) and got a BOGOF offer from me, clearly. That negated the need to return for a second day. More observations and blood tests ensure that you’re fit and well for discharge and that’s that.
In all honesty, the most painful part of the whole collection process was that my left arm (the one with the big needle) had seized up; getting movement back after the needle was removed was fun. Apparently the majority of harvests are done in one day and the majority of patients experience similar side effects to me, so this account, by all reckoning is representative.
I’ve mentioned before that the recipient is not in a good way; she currently has an infection which is preventing immediate transplant – Anthony Nolan will provide periodic updates on her progress which I shall pass on. In the meantime, if you’re between 16 and 30 and feel like signing up to the register to give someone the chance for life, you can do so here. If you’re older (or don’t want to – and there’s no shame in that whatsoever), then the charity’s work will benefit from any financial gift you can afford; there’s a Justgiving page here.
Finally, I should thank all of the staff involved at University College London Hospital and the Anthony Nolan Trust for their parts in all of this, along with the team looking after the recipient wherever they are in the world. Four people deserve a special mention though; Zia of the Anthony Nolan Trust for planning logistics and putting up with my ever changing diary without flinching; Penelope, the nurse that braved the Supreme Court and my stubbornness in relation to her orders of taking it easy, Maddie the nurse at UCLH that did most of the grunt work and has a surprising ability to stab you without you noticing and Daniel, the German specialist that finally got the big needle in and who has an uncanny interest in telecoms regulation!.

2 replies on “Donating Stem Cells (Part III)”
Well done mate – we are all proud of you:) LEts hope it helps her.
Second that, well done, and also well done for being so honest and telling it like it is, I am sure many brave youngsters will now come forward and help this worthy cause. I know I would after reading that if I was younger. It is a very NOBLE thing to do.
Kudos.
chris